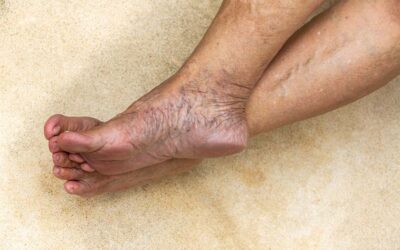
What causes varicose veins?
Prolonged standing can contribute to varicose veins. It puts increased pressure on the veins in your legs, causing the veins to dilate. In turn, valve cusps are pulled apart allowing blood to flow back down into the leg – resulting in the familiar appearance of knotted varicose veins.
Your body doesn’t actually need varicose veins
Once they’ve shut down or become abnormal, they do not return blood to the heart as veins are designed to do, as our body has already established alternative pathways to bypass them. They are not missed by your body’s circulatory system and once gone, it improves without them.
You’re more likely to get varicose veins if vein problems run in your family. If one parent has a vein disease you have about a 33 per cent chance of developing vein problems; if it’s both parents, this increases to a 90 per cent chance.
Signs and symptoms of varicose veins
Signs and symptoms of varicose veins include aching and heavy legs; tiredness; burning, itching and throbbing legs; night cramps; restless legs; ankle swelling; skin pigmentation; eczema; and ulcers. Vein disease is progressive so if left untreated, symptoms are likely to become worse and more serious complications such as phlebitis (inflammation of the vein), blood clots (such as deep vein thrombosis), dermatitis and vein ulcers can develop.
Preventing and Treating Varicose Veins
Wearing stockings or “skins” from a young age, particularly during excessive exercise or long periods standing, may help halt the progression and even development of varicose veins. Also the use of medical compression stockings or pantyhose may ease symptoms of varicose vein disease.
Modern non-surgical treatments are now available and proving popular for treating varicose veins. Treatments vary and can take as little as 30 minutes; most patients can walk in and out and return to their normal lives immediately. These treatments are effective and have a high success rate. They avoid the inconvenience of hospital admission, anaesthetic and potential scarring from surgery.
Non-surgical treatments include:
- Ultrasound Guided Sclerotherapy
Injecting a sclerosant solution into the abnormal veins (using ultrasound guidance), causing the vein wall to collapse. The veins dissolve and disappear as the body gradually absorbs them. - Microsclerotherapy
Injecting a sclerosant detergent solution through a tiny needle into the diseased vein, causing the vein wall to collapse. The veins dissolve and disappear as the body gradually absorbs them. - Endovenous Laser Ablation (EVLA)
The latest method for treating larger saphenous veins, previously treated by “stripping” surgery under general anaesthetic. It involves placing a laser fiber with ultrasound guidance into the abnormal vein. The vein is then numbed with local anaesthetic and the laser is activated and slowly withdrawn, resulting in obliteration of the saphenous vein along its entire length. - Ambulatory Phlebectomy
Eliminates varicose veins through a series of small punctures (as tiny as 1mm) made in the skin adjacent to the vein under local anesthetic. The varicose vein is then removed in small segments.
Be wary of miracle cures!
Be wary of miracle cures! There are many creams and herbal products not listed on the Australian Federal Government’s Pharmaceutical Benefits Scheme, which claim to help alleviate symptoms of varicose vein disease and even “make them disappear”.