- What are varicose veins and what do they look like?
- What are spider veins and what do they look like?
- Why do people develop varicose veins?
- Why are varicose veins bad for my health?
- What if I do not treat my varicose veins?
- Why do varicose veins appear in one leg only?
- Does crossing your legs cause varicose veins?
- What is a varicose veins specialist?
- Do I need these veins?
- Does it hurt to have varicose veins removed?
- Are topical skin lasers an effective treatment for spider veins?
- What type of solution is injected into veins?
- How many treatments will I require?
- Does the vein treatment interfere with my work or home duties?
- What should I expect after treatment?
- How soon after I get my veins treated can I fly?
- Can you tell me about exercise and my vein treatment?
- When will my varicose veins heal?
- Will the treated veins come back?
- What are the possible complications if I do not have any treatments?
- Should I wait until I have completed my family?
- Can I have treatment if I am pregnant or breastfeeding?
- What is the significance of me taking the oral contraceptive pill or hormone replacement therapy (HRT)?
- What are the costs of treatment?
- Does vein treatment require a stay in hospital?
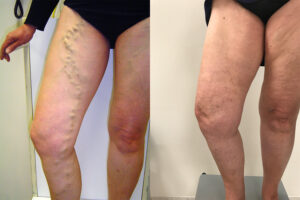
What are varicose veins and what do they look like?
Varicose veins are in the legs, they’re often large, lumpy, and bulge against the skin. In some cases, they can be dangerous and can result in skin changes, swelling, and ulceration.
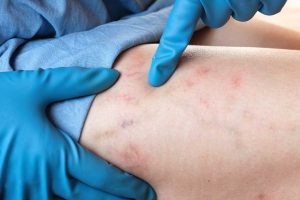
What are spider veins and what do they look like?
Spider veins are tiny red or purple veins that appear in clusters like a spider web. Spider veins can be the tip of the iceberg as approx. 20% of people with spider veins have deeper vein issues that should be treated in order to treat the spider veins.
Why do people develop varicose veins?
There’s a strong hereditary component to the development of varicose veins. If your parents have varicose veins, there’s a good chance you will have varicose veins too. It is also possible to develop varicose veins without a family history. In either case, it’s worth getting them checked out by a phlebologist.
Why are varicose veins bad for my health?
Despite popular opinion, varicose veins are not just a cosmetic concern. The pooling of blood within varicose veins can cause heaviness, tiredness, and discomfort in the legs. If left untreated, varicose veins can progress to skin changes and even skin ulceration. The best thing to do if you have varicose veins is to have them checked by a phlebologist and have them managed correctly.
What if I do not treat my varicose veins?
Vein disease is progressive which if left untreated is likely to become worse with time. Increasing symptoms that can occur with untreated varicose veins include leg tiredness, heaviness, aching, throbbing, restlessness, tingling, itching, numbness, and swelling. More serious complications such as phlebitis, blood clots, dermatitis, and vein ulcers can develop if varicose veins are left untreated.
Why do varicose veins appear in one leg only?
It is possible to get varicose veins in one leg only. However, a duplex ultrasound examination often reveals hidden varicose veins in the other leg also. To treat the visible varicose veins, we must also treat the deeper venous issues.
Does crossing your legs cause varicose veins?
No. There is no relationship between the way to sit and the development of varicose veins.
What is a varicose veins specialist?
A varicose veins specialist (or phlebologist) is a doctor who has gone through extensive training in the field of varicose vein disease and management.
Do I need these veins?
Varicose veins and spider veins are not functional. Once veins become abnormal, our body finds alternative pathways with healthy veins to carry blood. You can never run out of veins. Varicose veins are not missed by the circulation. In fact, it improves without them.
Does it hurt to have varicose veins removed?
The amount of discomfort felt will vary with the individual. The needles used are extremely fine (similar to acupuncture needles) and many are hardly felt at all. The injected solution can sting slightly for short periods of time. If EVLA is used, then minimal discomfort is experienced as it is performed under local anaesthetic.
Are topical skin lasers an effective treatment for spider veins?
Despite the proven usefulness in the treatment of large varicose veins using EVLA, the treatment of leg veins by laser light to the skin has thus far been disappointing. Currently, available lasers can be very useful in treating the tiny cosmetic facial veins but have been significantly less effective on leg veins when compared to expert sclerotherapy. Also, topical laser therapy is far from painless.
What type of solution is injected into veins?
The current recommended and TGA-approved solutions used for sclerotherapy in Australia are referred to as “detergent sclerosants”. Sodium Tetradecyl Sulphate and Polidocanol are the 2 detergent sclerosants used widely across the world. Hypertonic saline (concentrated salt water) has limited use in the treatment of varicose veins. Dr Paraskevas will discuss these sclerotherapy solutions in greater detail at the initial visit.
How many treatments will I require?
Your treatment protocol, which includes the number of treatments required, will be determined at your first consultation.
Does the vein treatment interfere with my work or home duties?
This is a walk-in, walk-out procedure. Most treatments take about 30 minutes to perform. Following treatment, your daily routine should not be disrupted, normal duties can be resumed.
What should I expect after treatment?
Most patients will experience some mild discomfort after the procedure, but nothing that will interfere with your daily routine. It is important to follow the post-procedure instructions carefully, which include walking, wearing a compression stocking, and drinking plenty of water.
How soon after I get my veins treated can I fly?
Flying for more than 4 hours within 3 weeks of varicose vein treatment with endovenous laser ablation (EVLA) or ultrasound guided sclerotherapy (UGS) should be avoided. There is an increased risk of in-flight deep vein thrombosis (DVT). Additionally, recovery and follow-up are important phases of healing. For flights shorter than 4 hours, patients can fly within 1-2 weeks after their treatment. However, it’s a good idea to follow the long-haul guidelines, as a precaution. Learn more about flying after varicose vein treatment here.
Can you tell me about exercise and my vein treatment?
It’s best to avoid heavy lifting and any strenuous activity for about 4-5 days after the treatment. This allows the body to recover after the procedure. It’s also important to walk 30 minutes a day.
When will my varicose veins heal?
Once treated, varicose veins can take many months to heal, varying from patient to patient. The good news is that relief from most symptoms comes quickly after treatment, generally within a few weeks.
Will the treated veins come back?
Treated correctly the veins will not come back, as the body has absorbed them. New veins, however, may appear with time. How quickly and how many appear, depends on whether you have inherited veins that are more likely to deteriorate. Other factors such as starting the pill, becoming pregnant, or occupations with prolonged standing, can affect the development of abnormal veins.
What are the possible complications if I do not have any treatments?
With large varicose veins, spontaneous blood clots may develop in the superficial veins and more rarely, the deep veins. Clots in the deep veins (deep vein thrombosis or DVT), can dislodge and travel to the lungs, which can cause pulmonary embolism, a life-threatening condition. Skin changes, including increased or decreased pigmentation, eczema of the skin (venous dermatitis), hardening of the skin and underlying fat (lipodermatosclerosis), and leg ulcers, may develop in the lower legs. Ulcers may become weepy, infected, and painful and take longer to heal.
Should I wait until I have completed my family?
Becoming pregnant with existing varicose veins will only lead to the veins becoming significantly worse as the pregnancy develops. Phlebologists agree that treatment for varicose veins is best performed before or between pregnancies.
Can I have treatment if I am pregnant or breastfeeding?
Sclerotherapy is best avoided when pregnant or breastfeeding. This is advised even though there is no current documented evidence to suggest that sclerotherapy is unsafe during pregnancy or breastfeeding. Vein treatments during pregnancy are not as effective often-producing poor results. It is recommended that sclerotherapy should be avoided if pregnancy is contemplated within the treatment course. Veins that appear during pregnancy should be treated before the next pregnancy to avoid deterioration with subsequent pregnancies.
What is the significance of me taking the oral contraceptive pill or hormone replacement therapy (HRT)?
Oral contraception and hormone replacement therapy-both oestrogen and progestogen have been implicated in increasing the risk of thrombosis whether you have a vein treatment or not. Taking the low dose contraceptive pill or HRT increases the risk of deep vein thrombosis 3 fold as compared to those not taking these products. Total correction of this increased risk requires ceasing hormone treatment for a minimum of 4 weeks. The increased risk seems to lessen the longer you have been on the medication. There is no current evidence that during sclerotherapy or EVLA treatment the taking of a low dose contraceptive pill or HRT actually increases the risk of thrombosis above the already existing risk before treatment. The relative merits of ceasing or continuing hormone therapy prior to sclerotherapy and EVLA treatment will be discussed further with you.
What are the costs of treatment?
The expected cost for treatment varies between individuals and will be provided in writing following your assessment. Rebate is claimable through Medicare except for the smallest spider veins. In Australia, the Medicare Safety Net reimburses eligible patients once a threshold has been reached. Please ensure that you are registered as a family or couple for the Medicare Safety Net.
Forms can be provided at your initial consultation or are available online at Medicare Australia. All payments are to be made on the day of review/treatment, by cash, EFTPOS, credit card, or cheque. Diners cards are currently not accepted.
Does vein treatment require a stay in hospital?
No hospital admission is necessary for our leg vein treatments. Sclerotherapy, ultrasound guided sclerotherapy, endovenous laser ablation, VenaSeal vein glue, etc – all these procedures are performed in clinic.