Varicose Veins Treatment > Ultrasound Guided Sclerotherapy
Ultrasound Guided Sclerotherapy
Ultrasound Guided Sclerotherapy (UGS) is a highly specialised procedure for treating advanced varicose veins that are hidden beneath the skin.
The procedure is very effective and involves injecting a sclerosant solution into the abnormal veins using ultrasound guidance, causing the vein wall to collapse. The veins dissolve and disappear as the body gradually absorbs them.
How does Ultrasound Guided Sclerotherapy work?
A detailed duplex ultrasound examination is carried out prior to the procedure to create a virtual map of the lower leg veins. This map precisely displays all abnormal veins, as well as adjacent structures such as deep veins and arteries, and helps the phlebologist identify the root cause of the visible varicose veins.
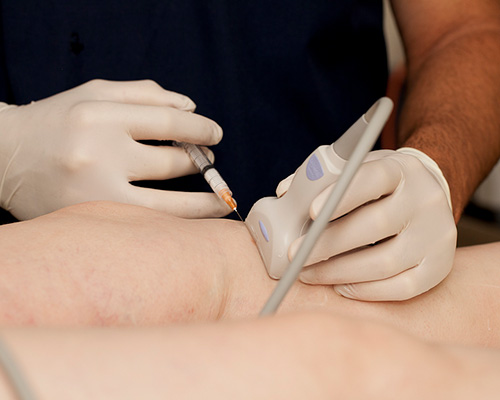
After the ultrasound, the patient lies comfortably on the treatment bed with the treatment leg exposed. With ultrasound guidance, the doctor can accurately guide the needle and inject the hidden abnormal veins, while observing the process on the ultrasound monitor. Once injected, the treated vessel will collapse and gradually be absorbed by the body, disappearing with time. A number of injections will be required along the length of the vein to achieve complete closure.
A significant advantage of this method is that it allows the phlebologist to monitor the effect of each injection, while ensuring the safety of all adjacent structures. The use of sclerosant as foam, rather than solution, has made this procedure much more effective.
What Happens After Treatment?
The treatment usually takes half an hour, but one hour is allocated to allow sufficient time for ultrasound examination, patient preparation, and discussion. Following the procedure, patients are fitted with grade 2 graduated compression stockings and asked to go for a 30-40 minute walk to promote blood flow into the deeper veins.
Patients are normally reviewed one week following the UGS procedure. At this review appointment, another detailed ultrasound is performed to ensure that the treatment was successful and any residual spider or varicose veins are injected using the microsclerotherapy technique.
Watch Sclerotherapy in Action
Further Patient Information Ultrasound Guided Sclerotherapy
What do I do Prior to Ultrasound Guided Sclerotherapy?
- Do not cease medications prior to treatment unless otherwise advised.
- Do not shave your legs immediately prior to your treatment.
- Do not apply moisturiser on the day of treatment.
- Wear slacks or loose trousers to the appointment and ensure you have a pair of comfortable walking shoes.
- Pre-medication is generally not necessary. If you have a low pain threshold, take 2 paracetamol tablets or 2 Ibuprofen tablets (with food).
- Treatment should be avoided if you intend to travel overseas within 3 weeks of your treatment.
- Treatment should be avoided for at least 2 weeks if you have returned from overseas travel.
- Patients who smoke should consider stopping before any treatment.
- Patients who are on the Oral Contraceptive Pill or HRT will generally be instructed to stop this medication prior to treatment. However, if this is not possible, Dr Paraskevas may prescribe a Clot Preventer that will help minimise the slightly increased risks of Deep Vein Thrombosis in patients who are taking these medications and who have Direct Vision Sclerotherapy.
What happens during Ultrasound Guided Sclerotherapy?
- An ultrasound probe will be used during the procedure.
- Ultrasound will help guide a fine needle into the hidden abnormal vein with extreme accuracy.
- Once the tip of the needle is inside the vein, a special solution known as a detergent sclerosant will be slowly injected into the vein. The solution will act locally to irritate the lining of the vein wall and subsequently collapse the vein shut. Over time, the treated vein will harden up and the body’s natural immunity will absorb it until it completely disappears.
- There are 2 types of Liquid Sclerosant available for use in Australia – STS and Polidocanol. When we inject larger veins with Ultrasound Guided Sclerotherapy, we use STS (Sodium Tetradecyl Sulphate). Clinically, STS is considered 3 times more potent than Polidocanol, which therefore makes its use for larger veins preferable.
What should you do after Ultrasound Guided Sclerotherapy?
- Class 2 compression stockings will be applied by our nurse.
- Our nurse will discuss all the important post treatment instructions in great detail and provide you with a post instruction sheet.
- You will be directed to go for an immediate 20-30 minute walk before you drive home.
- You will be given Dr Paraskevas’ after hours number should you have any problems or concerns.
- The stockings will be worn overnight for the first night.
- Following this, the stockings should be worn for a total of 14 days but only during the day. They can be removed for showering or when going to sleep at night.
- Walking for 30 minutes each day is mandatory.
- Maintain normal daytime activities but avoid standing still for long periods of time.
- Continue with normal exercise activities.
- You will be asked to avoid long haul flights (>4 hours of continuous travel) for at least 3-4 weeks after the treatment. If travel is unavoidable, then you will be protected from deep vein thrombosis with subcutaneous low molecular weight Heparin (aka Clexane) during your travel.
- An ultrasound check of the treated veins will occur 2 weeks after the treatment. This is to assess the outcome of the treatment and also to exclude the very low chance of deep vein occlusion.
What are some of the symptoms you can expect following Ultrasound Guided Sclerotherapy?
- Mild Discomfort. Patients may develop discomfort in the areas that have been treated. This may occur on the first day or may occur days or weeks later. It represents the hardening process occurring in the treated veins and the body’s mechanism of dealing with the dead vein. Discomfort is usually improved by walking or by taking Paracetamol or Ibuprofen. Soreness behind the knee can result from rubbing by the stocking. Soreness in the heel of the foot or in the toes indicates that the stocking is way too tight around the foot or ankle region.
- Bruising. Bruising usually disappears within 2-3 weeks and is not a cause of concern.
- Tender lumps. These are common in the treated veins and persist for the first few months. The lumps represent “hardened” or “sclerosed” veins – the precise intention of sclerotherapy. They will gradually reduce in size and eventually disappear. Sometimes, these lumps may contain “Trapped Blood” which is blood that has remained trapped within the “hardened” vein during the treatment. “Trapped Blood” can be gently drained by tiny pin pricks several weeks or months after the procedure.
- Pigmentation. Haemosiderin or Iron deposits from “Trapped Blood” blood can be deposited in the skin along the treated veins. This is more frequent with large surface veins but can occur with spider veins. Most disappear within 12 months but less than 5% can persist beyond 12 months. Persistent pigmentation may respond to laser treatment. Pigmentation may appear as light brown discolouration or as a dark shadow along the treated vein.
- Matting. This consists of networks of fine dilated capillaries near the injection sites. It appears shortly after treatment in approximately 10% of patients. Most resolve spontaneously. If there is Persistent Matting, there may be a vein that has not closed during the treatment. Meticulous Ultrasound Examination is extremely important right from the get to, to avoid areas of Persistent Matting.
- Phlebitis. Inflammation of the treated veins can occur during the healing process. It will appear as redness and tenderness over the “hardened veins”. Phlebitis must be reported to Dr Paraskevas but it is not serious and can be treated with oral Ibuprofen (Nurofen) and wearing the Class 2 Compression Stockings.
What are the possible complications from Ultrasound Guided Sclerotherapy?
Complications can occur even with the best possible technique and attention to detail.
- Deep vein thrombosis (DVT). Clots are a recognized complication of many procedures but are very rare with direct vision sclerotherapy if the protocol of compression and regular daily walking is followed. It is optional to stop hormone preparations (oral contraceptive or HRT) as they may increase the risk of DVT.
- Allergic reaction. This is rare but may present immediately as an anaphylactic reaction with generalised rash, constriction in the throat or difficulty with breathing. This is immediately treated by injecting cortisone or adrenaline. Allergy may cause a skin rash after treatment requiring antihistamines. Allergy is slightly more common in asthmatics. Patients must stay in the building for 10 minutes after any form of treatment to ensure that no allergic reactions occur.
- Intra-arterial Injection. Intra-arterial injection is a rare complication occurring when an artery, rather than a vein, is inadvertently injected with sclerosant. This causes the artery to spasm and sclerose, resulting in severe tissue necrosis in the area the artery supplies. Limb amputation can occur as a result of this necrosis unless this complication is identified and treated promptly.
What standards and guidelines are in place for practitioners of phlebology?
Medicare Rebate & Costs
The cost of treating varicose veins depends on severity of the veins as well as which treatment is used. We discuss these costs in detail at your initial consultation.
A Medicare rebate is claimable on all varicose vein procedures, except the most superficial spider veins.

What to expect
Learn all about your first appointment, what's included, and how much it will cost.
