If you want to make sure you get the best treatment for varicose veins, here’s what you need to know to identify excellent quality care for venous disease. That means you can make an informed decision about your treatment and understand the steps we take to maximise your chances of an excellent treatment outcome.
You should be given a comprehensive initial assessment.
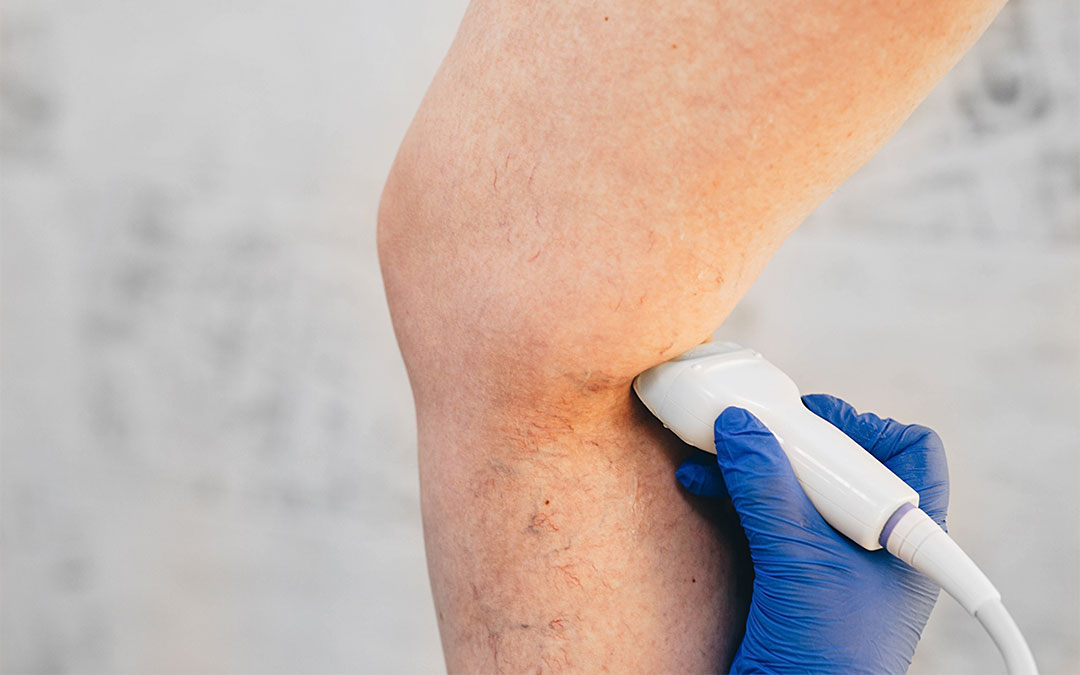
An initial assessment of suspected varicose or spider veins involves a careful comprehensive examination. It should include the patient’s medical history, physical examination, and a duplex ultrasound to identify the source of any vein abnormalities.
Some doctors and surgeons who assess for vein irregularities either neglect to perform an ultrasound, are not experienced or trained on ultrasound for veins specifically or outsource ultrasound to an external sonographer or radiology department without any specialisation in veins either.
If underlying veins are not mapped out correctly, the veins that are the origin of the problem will remain unidentified and go untreated. That means your varicose veins will come back.
Treating phlebologists (vein doctors), doctors, or surgeons should be experienced with vein treatment.
Successful treatment will come from a doctor who has undergone years of training in vein disease, has successfully treated many patients, and has kept up to date with treatment innovations and technology, so they will be able to expertly treat all forms of vein disease. This may include pregnancy-related and pelvic veins, persistent embryonic veins, venous insufficiency, malformations, and chronic & severe vein disease. These are not just cosmetic concerns; you need to be treated by someone who will take a comprehensive approach to your overall health as well as your veins.
Dr Paraskevas has been treating varicose veins for approaching two decades and is a Fellow and Board Member of the Australasian College of Phlebology. It is important for referring doctors and patients to know that the Australasian College of Phlebology is an internationally recognised vein college that provides comprehensive training and assessment to doctors in the field of Phlebology.
You should receive the right treatment for you.
As physicians and surgeons, our patient’s safety and long-term health are our priority. As per the NICE Guidelines, Dr Paraskevas performs the latest non-surgical, minimally invasive techniques for varicose vein disease. Each presentation of venous incompetency is different, and for each our phlebologist selects the ideal minimally invasive varicose vein treatment based on vein diameter, location, and severity. After our treatments, patients are encouraged to walk straight away, as well as for 30 minutes per day, and will wear compression stockings for two weeks during the day.
Minimally invasive techniques such as endovenous laser ablation, radiofrequency ablation, VenaSeal medical glue, and ultrasound guided sclerotherapy are alternatives to traditional surgery. Each treatment has its intended use; for example, endovenous laser ablation is the preferred method for treating an incompetent great saphenous vein as it provides a more definitive result as compared to sclerotherapy. The treating doctor should be able to discuss the advantages and disadvantages of each treatment and how they will be applied to your specific problem.
Feeder veins should be treated before spider veins.
Just like failing to map out veins on ultrasound, if your doctor or surgeon only treats visible veins on the surface, such as fine spider veins without treating the feeder veins (reticular veins), the appearance of the skin surface and painful symptoms will get worse.
Patients sometimes tell us they have had sclerotherapy in the past, but it “didn’t work” because the spider veins came back. However, what has often occurred is the underlying veins have not been treated first, fine capillaries known as matting develop, and new spider veins bloom on the surface of the skin.
In our clinic, we treat feeder veins first and spider veins second, usually several weeks apart.
Follow-up is important.
All treatments should be followed up to confirm that the treatment was effective. In our clinic, all patients have mandatory follow-up visits after treatment. Patients are placed on a long-term follow-up regime, at 12 and 24 months, to ensure that the successful outcomes are maintained.
Key Takeaways
- Patients should receive a comprehensive initial assessment, including an ultrasound.
- Treating phlebologists should be experienced in treating veins
- You should have a non-invasive treatment performed that is tailored to your condition.
- Underlying feeder veins should be treated before spider veins, not just the surface veins alone.
- Receiving follow-up care is important for successful treatment.