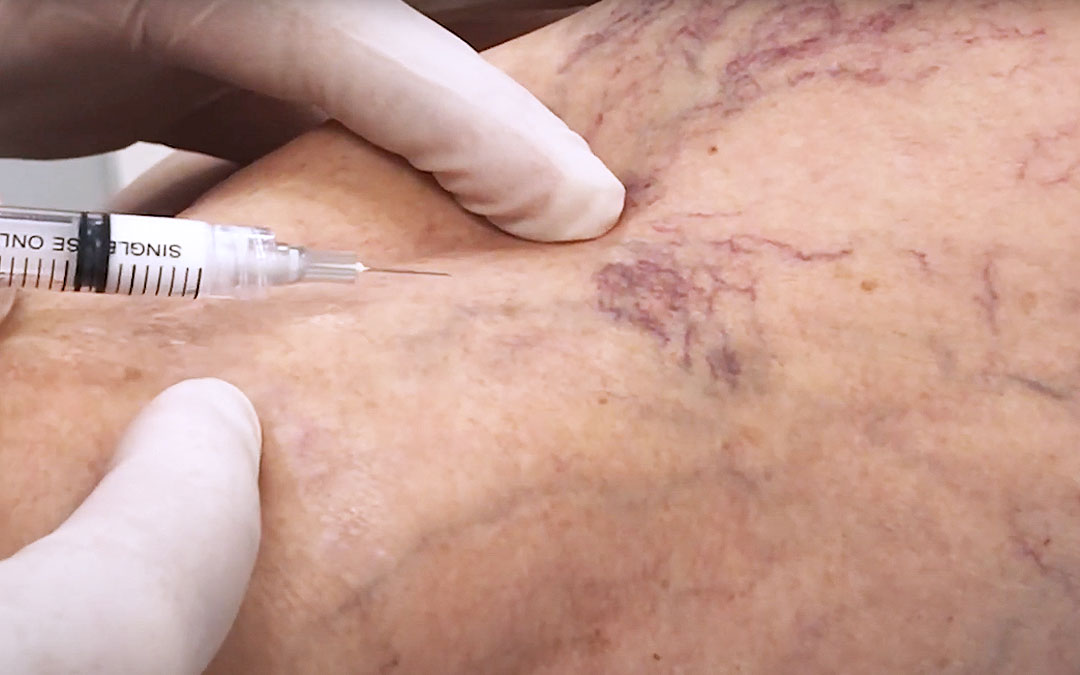
Hyperpigmentation is a darkening of the skin. It is a symptom of conditions in several different regions of the body. There are a couple of reasons why it is relevant to varicose veins, healing from sclerotherapy and a symptom of serious venous disease. It might look like a light brown discolouration or a dark shadow near the area of the vein.
A quick note on terminology: Pigmentation refers to skin colour or the amount of melanin in the skin. Sometimes pigmentation and hyper-pigmentation are mistakenly used interchangeably to refer to discolouration or darkening of the skin. But for our purposes, we’ll be using the term hyperpigmentation for staining or darkening of the skin’s normal pigment.
What has hyperpigmentation got to do with varicose veins?
Hyperpigmentation after sclerotherapy or due to chronic venous disease is often referred to as haemosiderin staining. Hemosiderin is a protein that stores iron in our blood and tissues and can accumulate in the blood under certain circumstances. The word siderin is Greek for iron. Once accumulated, it can cause brown or black staining or a bruise-like appearance.
Haemosiderin is a broken-down product of haemoglobin found in red blood cells and carries oxygen around the body. When red blood cells die following vein treatment or due to severe varicose veins, haemoglobin is released into the tissues and breaks down into haemosiderin (iron). The haemosiderin is then deposited into the skin, causing visible hemosiderin staining.
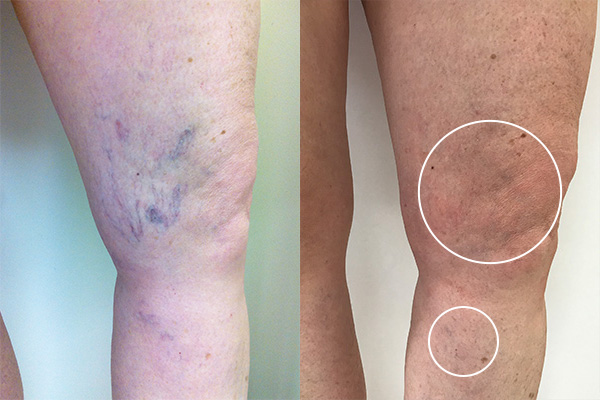
Before and after sclerotherapy. After image shows faint hyperpigmentation (circled).
Hyperpigmentation during post-sclerotherapy healing
This is part of the normal healing process that takes place after sclerotherapy treatment. During sclerotherapy, spider and varicose veins are injected with a solution that irritates the interior vein wall, making it collapse on itself, harden, and the body slowly absorbs it over time. A small amount of blood may become trapped in the vein as it is treated. As the body breaks the vein down, some of this haemoglobin within the blood is released into the skin and is broken down into haemosiderin. Haemosiderin is then deposited into the dermis, discolouring the skin as the treated vein heals.
What is considered successful sclerotherapy?
When spider veins or varicose veins have been successfully treated by sclerotherapy, including ultrasound guided sclerotherapy, they may darken at first. If you apply pressure to the veins, they won’t blanch – i.e., pushing blood away and then it flows again. If they look like darkened threads even when you press them, this hyperpigmentation shows the treatment has been successful. The vein has been sealed up and no blood flow is continuing through the vein and the healing process can begin. And don’t worry, you don’t need diseased veins that are no longer performing their job. We never run out of healthy veins because the body finds alternative pathways to carry blood.
Normal Post Sclerotherapy Hyperpigmentation (Physiological Pigmentation)
Post-sclerotherapy, some patients may notice hyperpigmentation occurs especially with large surface leg veins, but sometimes spider veins too. White blood cells (or cells from the immune system) begin to break down and absorb the dead vein and any trapped blood after treatment. Any haemosiderin deposits are then dealt with by the body’s immune system and gradually disappear with time. Within 6-12 months, most of this hyperpigmentation will heal up. Less than 5% continue beyond 12-months. If there is any persistent discolouration, it may respond to laser treatment to restore normal pigmentation, although we have never had to resort to this in our 17 years of practice.
Although staining following this treatment is considered a normal part of the healing process and is not a failure of the treatment, good technique by the treating doctor can help reduce the risk of hyperpigmentation. Avoiding high concentrations of solution and high plunger pressure prevents aggressive damage to the vein. After the sclerosant is injected, compressing the vein by hand can help close it and prevent it from refilling, avoiding trapping too much blood which causes hyperpigmentation. Seeing an experienced phlebologist is vital in reducing the chances of post sclerotherapy hyperpigmentation.
Abnormal Post Sclerotherapy Hyperpigmentation (Pathological Pigmentation)
This occurs because of inadequate treatment, where there are leaky veins still left behind after venous sclerotherapy. Blood is rerouted directly into segments of abnormal vein or capillaries that store the blood and release it periodically into the skin. This is broken down and stored as iron. This kind of skin discolouration will never go away without intervention. It requires a thorough assessment with duplex ultrasound to find where the leaky blood is coming from and to fix it correctly. To avoid this, careful ultrasound diagnostic assessment at the initial consultation is crucial, followed by a thorough treatment of varicose veins and capillaries.
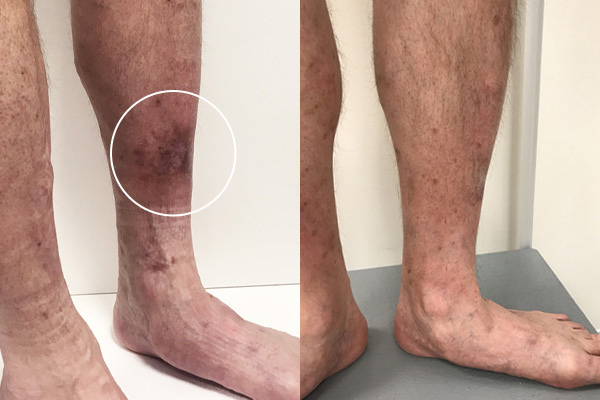
Before and after pictures of legs with severe hyperpigementation from chronic venous disease. Photo from before treatment shows hyperpigmentation (circled).
Hyperpigmentation, a symptom of severe varicose veins
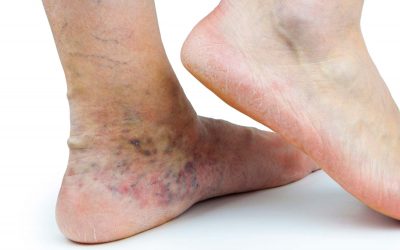
This staining can occur where a severe varicose vein under high pressure pushes blood into fine surface capillaries. As the capillaries become more and more engorged, red blood cells and haemoglobin are pushed into the skin, where they are broken down into haemosiderin (iron), staining the skin. This hyperpigmentation can become dark and even after successful treatment of the venous insufficiency, may never fully disappear. Fortunately, the staining does lighten somewhat after treatment.
Severe varicose veins and hyperpigmentation
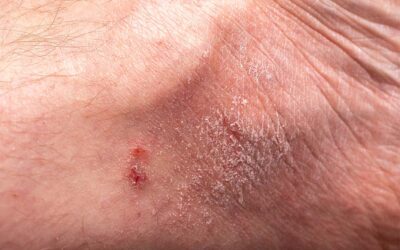
When severe varicose veins are the cause of darkening or staining of the surface, there is reason to pay attention. This can indicate progressive venous disease. Other symptoms that may accompany chronic or severe venous disease may include venous eczema/venous dermatitis, oedema (swelling of the leg), phlebitis and cellulitis, lipodermatosclerosis (thickening of the skin of the lower leg or ankle), a venous ulcer (the breakdown of skin), and thrombophlebitis. In cases like this, a phlebologist should perform an examination and ultrasound to diagnose any problem veins or venous disease.
Key takeaways
- Hyperpigmentation related to varicose veins may be caused by severe varicose veins or recovery from sclerotherapy treatment.
- When recovering from sclerotherapy, it is normal to expect some discolouration of the skin as the treated leg vein heals and is reabsorbed into the body, but staining is unlikely to be permanent.
- Abnormal pigmentation or persistent hyperpigmentation following treatment may be a sign the initial duplex ultrasound assessment and treatment was inadequate. Seeing an experienced phlebologist may help mitigate these risks.
- Hyperpigmentation is also a symptom of serious venous disease which should be assessed by a phlebologist.