Varicose Veins
Healthy veins carry deoxygenated blood toward the heart, against gravity. Varicose veins in the legs or groin are defective and can no longer transport blood back to the heart effectively. This is also known as venous insufficiency or incompetency.
Healthy veins have stepped one-way valves along their inner walls which allow blood to flow in one direction only. The valves close between heartbeats to stop backflow. When these valves fail, the blood leaks backward, increasing pressure inside the vein, expanding its width, becoming visible on the skin surface, and causing a range of symptoms.
Symptoms
Varicose veins can range from small thread-like veins called spider veins (or telangiectasia) to slightly larger blue veins or reticular veins, to large and bulging varicose veins. Varicose veins can affect any part of the leg or pelvic area.
Symptoms may indicate that you have vein problems in your legs or groin. Keep in mind that you may be more aware of these signs in the evening/night or at the end of a long day of sitting or standing still.
Common varicose vein symptoms
- Swelling in the legs
- Localised pain and aching in the legs, may be tender to touch
- Leg fatigue and heaviness
- Burning, itching (For more, see: Why are my varicose veins itchy?)
- Throbbing
- Unexplained cramping
- Restless legs (For more, see: Restless Legs at Night)
Severe varicose vein symptoms
These symptoms can indicate advancing vein problems.
- Skin rashes
- Small blue veins on the feet (For more, see: Are ankle and foot veins linked to deeper vein problems?)
- Venous eczema (For more, see: Venous Dermatitis: Untreated Varicose Vein Complications)
- Swelling of the leg
- Hyperpigmentation – Discolouration of the skin
- Inflammation
- Leg ulcers/open sores (For more, see: Why are venous leg ulcers so hard to heal?)
- Lipodermatosclerosis – Thickening of the skin of the lower leg or ankle (For more, see: What is Lipodermatosclerosis?)
- Phlebitis and Cellulitis – Severe bacterial infection of the vein and the surrounding tissues below the skin.
- Thrombophlebitis – Superficial thrombophlebitis or deep vein thrombosis (DVT). (For more, see: 3 Causes of Deep Vein Thrombosis)
Varicose veins may present as
- Prominent veins alone – visible, bluish, and bulging varicose veins, smaller thread-like spider veins, or reticular veins with no notable other symptoms (eg: no swelling or throbbing).
- Prominent veins and symptoms – visible, large, bulging varicose veins with pain, swelling, itching, etc.
- Symptoms alone – Symptoms (eg: pain, swelling, throbbing, etc) with no visible abnormal veins.
Causes
Varicose veins affect about 30% of women and men of all ages (but commonly between 34 and 64 years of age.) Women may experience vein problems earlier in life than men.
The conclusive cause of varicose veins is not known but risk factors for developing varicose veins and venous disease are:
- Genetics – a strong family history of varicose veins is an indicator you will have them too.
- Occupations requiring prolonged standing/sitting/immobility.
- Hormonal fluctuations – adolescence, birth control pills, pregnancy, menopause, etc.
- Previous blood clots
- Leg injury
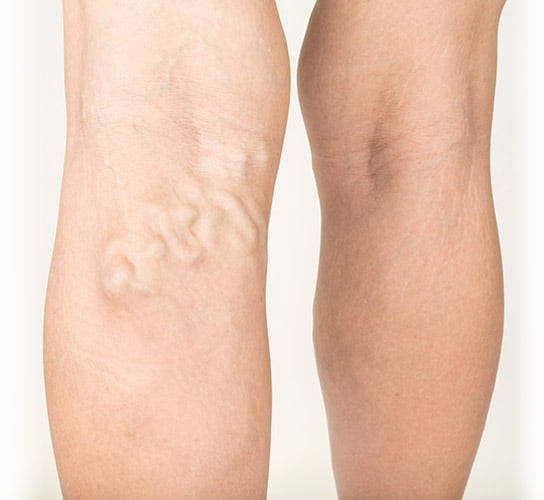
Moderate Varicose Veins
These large, dilated, ropey veins that bulge above the skin surface, and are usually blue or green in colour. They no longer serve the primary function of veins, which is to return blood to the heart. Varicose veins can occur alone or with many of the physical manifestations of chronic venous disease. Many patients do not realise they have a complication of venous disease until they see a phlebologist (vein doctor).
What are the symptoms of moderate varicose veins?
The signs and symptoms of moderate varicose veins may include aching and heavy legs, tiredness, burning, itching, and throbbing.
Some patients may present with none of these symptoms, and may feel that there is nothing wrong with the affected leg. However, there can be real medical consequences to leaving varicose veins untreated. This can be a progressive condition and new faulty veins can develop with time, along with worsening symptoms and complications.
How do we treat Moderate Varicose Veins?
Moderately severe varicose veins can be treated non-surgically with a combination of Endovenous Laser Ablation and Sclerotherapy using Ultrasound. Some doctors may also perform Modified Ambulatory Phlebectomy for any larger problem veins.
Vein Health Medical Clinic’s treatments are deemed to be safe and effective procedures. These varicose veins treatments do not require general anaesthetic or hospital admission, and avoid the potential scarring effects of surgery. In the past, an in-hospital stay for surgery was necessary, but now patients can walk-in, have varicose veins treated in less than an hour, and walk out. No downtime from work is required; patients can return to normal duties immediately.
Dr Paraskevas performs non-surgical treatments of varicose veins of all levels of severity.
Endovenous Laser Ablation (EVLA)
Under ultrasound guidance, a laser fibre is placed into the abnormal vein through a tiny incision. When the laser is activated and the fibre is slowly removed, this produces a reaction in the vein wall along the treated section, resulting in collapse and sclerosis of the vein wall with minimal discomfort.
Ultrasound Guided Sclerotherapy
Ultrasound Guided Sclerotherapy is a highly specialised procedure involving injecting a sclerosant solution into the abnormal veins using ultrasound guidance, causing the vein wall to collapse. The veins dissolve and disappear as the body gradually absorbs them.
Radiofrequency Ablation
Radiofrequency ablation (RFA) relies on thermal (heat based) damage to the vein, that leads to immediate closure of the vein. Once the vein is treated by radiofrequency ablation, it will gradually undergo complete absorption by the body and disappear over time.
Conditions
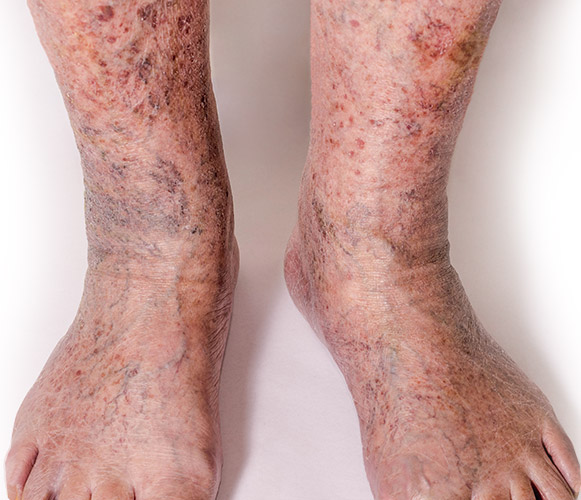
Severe Varicose Veins / Chronic Venous Disease
Venous disease is a progressive condition. It will not improve or go away by itself. As time passes, there will be an increasing number of varicose veins, spider veins, and other painful symptoms that will worsen. It can develop into the breakdown of the skin, open sores that won’t heal, and even blood clots.
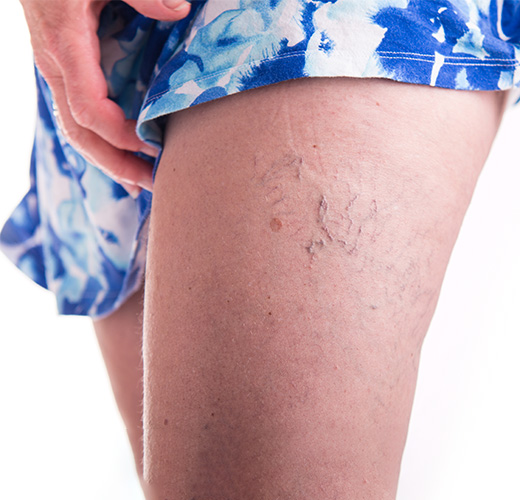
Spider Veins and Reticular Veins
Spider veins are the tiny red or blue veins that can appear anywhere on the body, but more often on the legs, ankles, face, chest, or abdomen. Spider veins are extremely common. They may appear to be short, seemingly unconnected lines, each about the width of a large hair, or they may resemble a spider web or a tree with branches. In medical terms spider veins are called telangiectasias, and usually occur in association with larger dilated blood vessels (often blue / green in colour) called reticular veins. Often dilated blood vessels cause aching especially with prolonged standing.
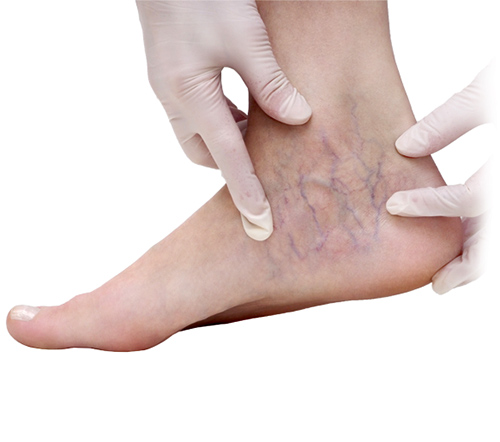
Feet and Ankle Varicose Veins
Spider veins or varicose veins that appear around the ankle or foot are known as Corona Phlebectasia by medical professionals. Etymologically, ‘corona’ refers to fan-like rays that radiate from the sun’s surface and, in this medical context, describes the fan-shaped nature of spider vein capillaries on the inside of the foot. ‘Phlebectasia’ indicates the presence of abnormal veins and capillaries. Together these terms refer to a fan-like spread of abnormal capillaries.
Pelvic, Vaginal, and Vulvar Varicose Veins
Pelvic, vaginal, and vulvar varicose veins occur in and around the groin area and can be worsened (exacerbated) following previous treatments including laser or radio frequency ablation, sclerotherapy or surgical ligation (with or without stripping) of the sapheno-femoral junction or can also occur after multiple pregnancies, and in some cases after one pregnancy. They can be present with or without accompanying symptoms.
Can Pelvic, Vaginal, and Vulvar Varicose Veins be Treated?
Pelvic, vaginal and vulval varicose veins can be treated quite effectively with ultrasound guided sclerotherapy. This procedure is performed by experienced senior phlebologists. It requires the use of advanced ultrasound equipment and careful isolation of the pelvic veins. As with lower leg varicose veins, the treated veins will undergo a hardening process referred to as sclerosis and will eventually get absorbed by the body. Once these veins have been treated, any congestion or symptoms associated with the build-up of blood within them, should resolve.
Can Varicose Veins in the Groin Region Occur in Men?
Yes. It is not just women who suffer from varicose veins of the groin area. Doctors report men can also suffer from pelvic varicose veins.
When Should You Seek Treatment?
Regardless of the location of the varicose veins, whether in the pelvic region or in the thighs, legs or ankles, getting the appropriate treatment from an experienced phlebologist is important. Treatment will help relieve symptoms and prevent further deterioration of vein disease.
For patients who are currently pregnant, it is appropriate to recommend treatment between pregnancies. Treatment during pregnancy is not recommended. In our experience, varicose veins in the pelvis and legs should be treated before the next pregnancy to avoid deterioration with subsequent pregnancies.
Varicose Vein FAQ’s
Who is affected by varicose veins?
Varicose veins usually run in the family. If one parent has had venous disease you have about a 33% chance of developing vein problems; with both parents this increases to about 90%. Contrary to popular belief, both men and women are affected. It may be noticed earlier in women as symptoms can be exacerbated by pregnancy.
Do I need to treat varicose veins? Isn’t this just cosmetic?
Many patients complain about their varicose veins being ugly – however, we need to be clear, we are dealing with a medical issue that can become worse over time, and lead to complications. Learn more about how varicose veins are more than just cosmetic.
How can I prevent varicose veins?
Patients who have varicose veins are predisposed to developing them at birth. The best thing to do to manage them conservatively (in other words, without having any treatment) is to ensure that you get enough rest, eat a healthy diet, and keep your weight down. This will help your overall health, including your veins. Learn more about how to prevent varicose veins.
Do you still need those veins?
Varicose veins are no longer serving a useful function to circulation. In fact, when the vein becomes defective, the body develops alternative pathways and bypasses the varicose vein altogether. You will never run out of alternate pathways. When a phlebologist closes down a varicose vein, the circulatory system improves, as do many of the symptoms. The problem veins will not resolve themselves without medical intervention.
Varicose Vein Recurrence: Will treated varicose veins come back?
Not the same ones, no. However, there are three reasons varicose veins can recur. One, the progression of venous disease. Not a one-off problem for many, venous disease will continue to progress over a lifetime, so new varicose veins can develop. Secondly, inadequate diagnosis where the origin or feeding veins are not identified so new problem veins spring from this source. And finally, neovascularity following vein stripping surgery is a complication of the surgery where primitive blood vessels develop inside the upper thigh area of the leg and the groin. Learn more about varicose vein recurrence here.
How do phlebologists classify the severity of venous disease?
In the past, it has been tricky for phlebologists and health professionals to define vein disorders because of the range and severity of symptoms. By creating the CEAP venous disease classification system, the discussion of conditions and treatments is standardised across the world. Read more about the CEAP classification system.
Other Vein Conditions
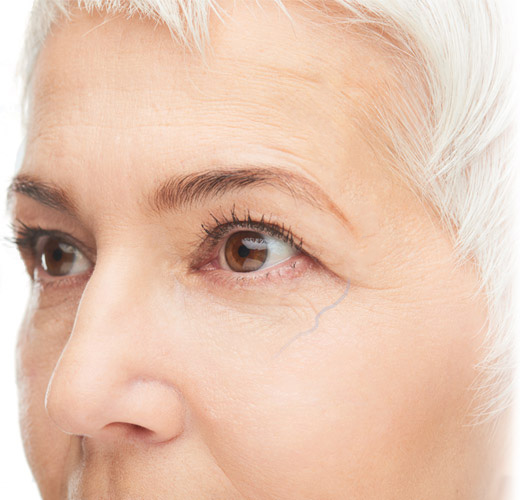
Periorbital Veins
Periorbital veins (POV) are often a cause of cosmetic concern for patients. POVs are superficial veins which start at the bridge of the nose and stretch below or above the eye to join venous branches on the lateral forehead and scalp. Under normal circumstances, periorbital veins are barely visible to the human eye.
Recent Vein Articles
What Is Chronic Venous Insufficiency?
Chronic Venous Insufficiency (CVI) is when the leg veins can’t efficiently return blood to the heart due to valve problems, causing pooling, swelling, discomfort, skin changes, and sometimes ulcers.
Walking and Exercise After Vein Treatment
Walking 30 minutes daily post-treatment is key to your recovery. Discover which exercises to embrace or avoid to ensure optimal healing and long-term vein health.
Night Cramps and Varicose Veins: Is This Keeping You Awake?
Many people experience leg cramps and discomfort at night, but few realise these symptoms might be linked to an underlying venous condition.
Medicare Rebate & Costs
The cost of treating varicose veins depends on severity of the veins as well as which treatment is used. We discuss these costs in detail at your initial consultation.
A Medicare rebate is claimable on all varicose vein procedures, except the most superficial spider veins.

What to expect
Learn all about your first appointment, what's included, and how much it will cost.



