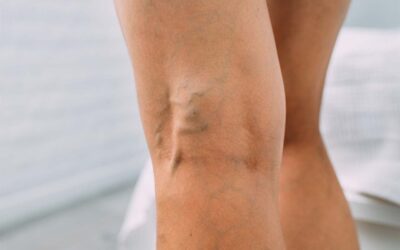
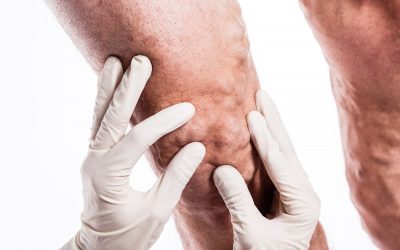
Pelvic congestion syndrome (PCS) is a condition affecting 2-7% of women who have been pregnant but also occurs in women who have not been pregnant. Varicose veins develop in the pelvic region, below the abdomen, and are often not visible on the surface of the skin, like we traditionally think of varicose veins. It sometimes begins with venous insufficiency of the ovarian veins. This is where the valves inside the veins are damaged and blood has reverse flow and pools there, causing an aching pressure, pelvic pain, or throbbing. So, is that just period pain or pelvic congestion syndrome?
Symptoms
The symptoms of pelvic congestion syndrome vary between women and often have some cross-over with other conditions many women experience. One of the most common is a dull ache or throbbing pelvic pain which worsens: in the late stages of pregnancy, in the days before getting your period, after prolonged standing, or during and after sexual intercourse.
In addition to pelvic pain/throbbing, here are the symptoms women also report:
- painful periods
- abnormal bleeding during menstruation
- visible varicose veins around the vulva, buttocks, and legs
- swelling of the vagina or vulva
- abnormal vaginal discharge
- frequent urination
- irritable bowel symptoms
- aching back and/or hips
- depression
- fatigue
- tenderness of the abdomen
The cause of pelvic congestion syndrome
Risk factors that may contribute to pelvic congestion syndrome are:
- A genetic predisposition to varicose vein and spider veins.
- Elevated levels of estrogen. Eg: this condition rarely appears after menopause.
- Pregnancy – Fluctuations in pregnancy hormones may weaken the valves in the veins, or additional fluid and pressure placed on the veins in the pelvis by the growing baby.
- PCS can occur without pregnancy, but with the contributors common to vein disease found in the legs: advancing age, obesity, prolonged standing or sitting, immobility, lack of exercise, and obesity.
Pelvic congestion syndrome can be difficult to diagnose. It may be written off as just period pain or pregnancy discomfort and may not be identified until afterward. After pregnancy, the veins will not repair themselves, but the pain may reduce slightly, as the baby is no longer contributing to the pressure on the problem veins. However, the veins will likely continue to develop and may appear on the thighs and legs. The pelvic pain and swelling from these veins are often what motivates patients to present at our clinic.
When post-pregnancy leg veins are investigated by our phlebologist with an ultrasound examination, the origin of the veins is frequently found to be in the pelvic region. Finding this is good news, as it means the source of the varicose veins can be treated, not just the effect. If we treat just the visible veins and not the veins that can’t be seen with the naked eye, they will return.
How is it treated?
When pelvic congestion syndrome is suspected, a phlebologist (vein doctor) will carry out an examination, medical history, and abdominal and vaginal ultrasound to accurately diagnose and define treatment.
There are three methods of treatment for the veins in the pelvis and groin: surgical ligation (surgically tying off the vein), ovarian vein embolization (cutting off blood supply endoscopically), and sclerotherapy (sealing the vein closed, minimally invasive). In our clinics, we use the most conservative option, which is ultrasound guided sclerotherapy, which enables the treatment of the problem veins with the least invasive technique, and it requires no hospital stay. It gives excellent symptom resolution and follow-up scans usually show no signs of venous reflux.
For the varicose veins on the lower legs and thighs which have their origins in the incompetent pelvic veins, we may use a combination of sclerotherapy, endovenous laser ablation, radiofrequency ablation, or VenaSeal medical glue, depending on the diameter and severity of the veins.
Key takeaways
- Pelvic congestion syndrome is when the faulty valves in ovarian and pelvic veins allow reverse blood flow in the veins.
- PCS may be caused by a family history of varicose veins, elevated estrogen levels, changes from pregnancy, and any factors that cause venous disease in the legs like immobility, obesity, etc.
- Further reading: Check out this case study/article written by our own phlebologist Dr Peter Paraskevas published in Phlebology magazine – Successful ultrasound-guided foam sclerotherapy for vulval and leg varicosities secondary to ovarian vein reflux: a case study