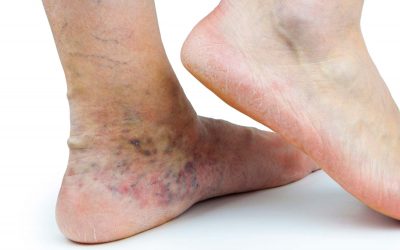
Varicose Veins are a component of a broader medical condition known as Chronic Venous Disease (CVD). Similar to other chronic conditions, the initial stages of CVD are often mild and go unnoticed as a threat to the patient’s well-being. However, as the disease progresses, complications can arise, significantly impacting the patient’s health in the long term.
For instance, individuals in the early stages of Type 2 Diabetes may not experience any symptoms apart from elevated sugar levels. The same can be said for those with high blood pressure, which is incidentally discovered during a medical visit to their GP. If left unaddressed, these conditions can lead to serious complications such as heart attacks, strokes, kidney problems, and heart failure. As the condition advances, it begins to affect other parts of the body in an adverse way.
Similarly, patients with progressive Varicose Veins who do not receive timely treatment will notice additional signs and symptoms stemming from the underlying vein problem. These untreated Varicose Veins can worsen, leading to complications like lower leg swelling, skin changes, thickening and degradation of soft tissue, and even ulceration.
As Phlebologists, we conduct routine duplex ultrasound examinations on all patients with Varicose Veins to evaluate the severity and likelihood of progression to a severe disease state.
Patient Case Study
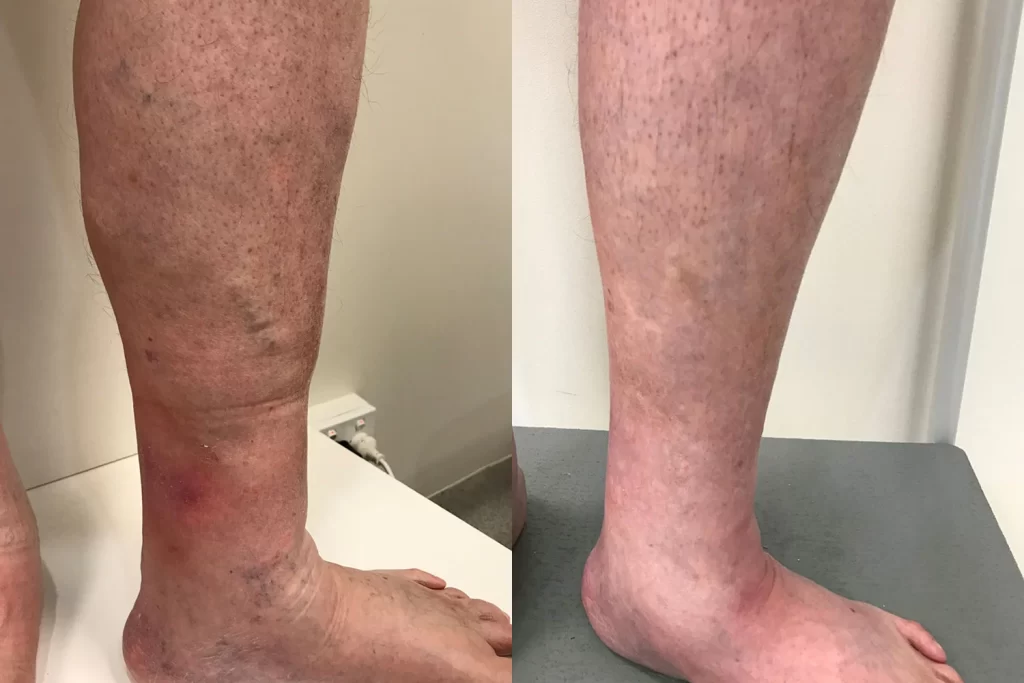
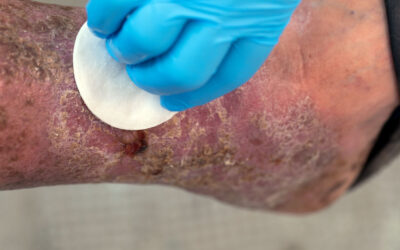
The image here shows the consequences of advancing venous disease. In this case, a 78-year-old man with chronic venous disease. He presents with varicose veins in the left lower leg, peripheral oedema (swelling), and Lipodermatosclerosis (hardening/thickening of the soft tissue in the lower leg). Notably, the swelling obscures the severity of the chronic skin and soft tissue damage taking place here. The redness in this area signifies acute inflammation of the skin and soft tissue, which can complicate the Lipodermatosclerosis (often referred to as Chronic Panniculitis) and can act as a precursor to Venous Ulceration (leg ulcers).
Remarkable Improvements
After undergoing Endovenous Laser Ablation and Ultrasound Guided Sclerotherapy at our clinic, the patient experienced a profound improvement in the health of the skin and soft tissue. The post-treatment photos taken at 18 months, with the swelling reduced, now reveal the presence of the underlying soft tissue necrosis, degradation, and micro-ulcerations known as Atrophie Blanche, which Phlebologists associate with venous hypertension.
What is Atrophie Blanche?
This condition manifests as small porcelain-white scars resulting from skin micro-infarction in an area affected by venous hypertension, caused by the obstruction of dermal arterioles and subsequent infarction (death of the tissue due to obstruction of the blood supply) of the skin supplied by these blood vessels.
Prompt diagnosis and treatment of Varicose Veins can help prevent many of these complications.
Key takeaways:
- Varicose Veins are just one aspect of a larger issue and can often lead to Venous Hypertension.
- Complications associated with Varicose Veins include swelling (oedema), Venous Dermatitis, Pigmentation, Lipodermatosclerosis, and Skin Ulceration.
- Atrophie Blanche indicates advanced venous disease changes.
- Prompt diagnosis and treatment of Varicose Veins can help prevent many of these complications.