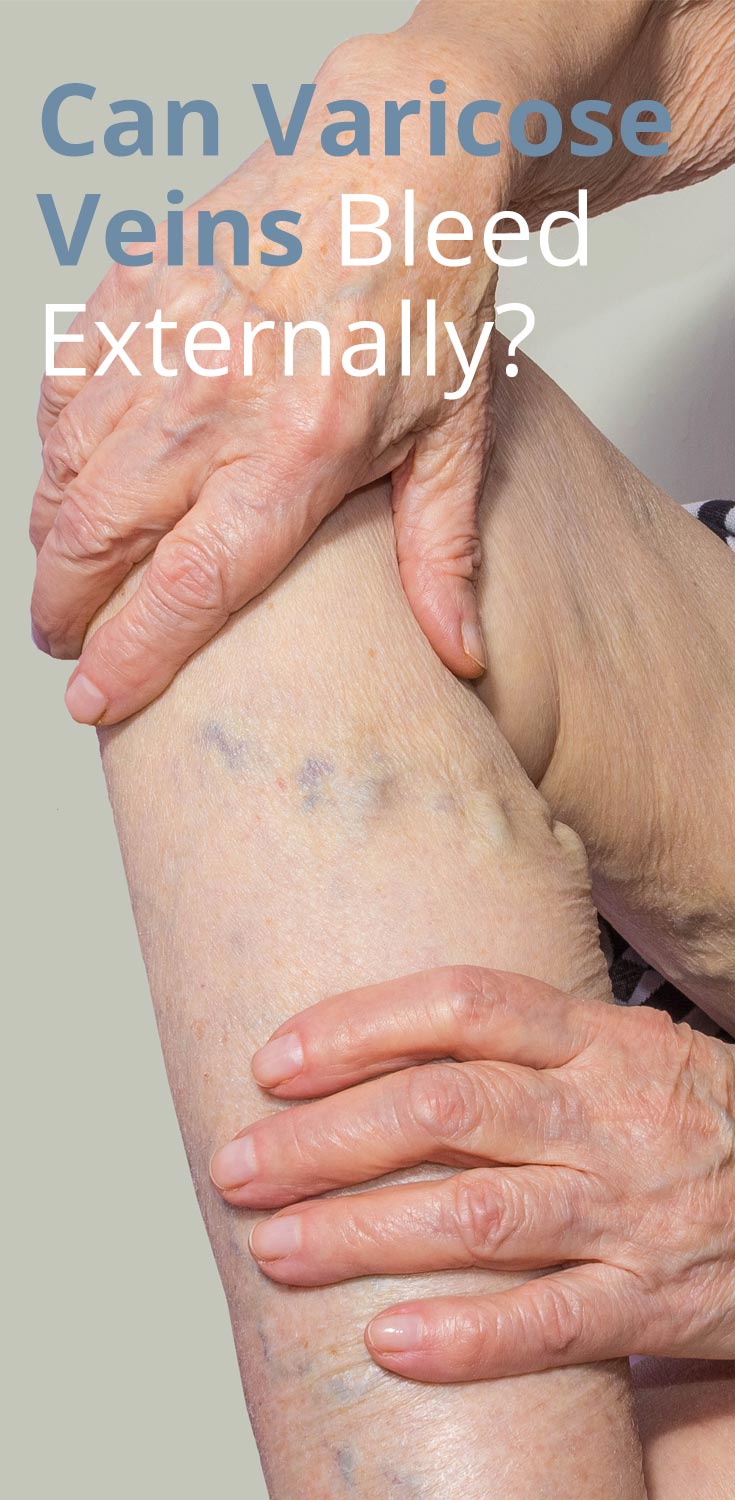
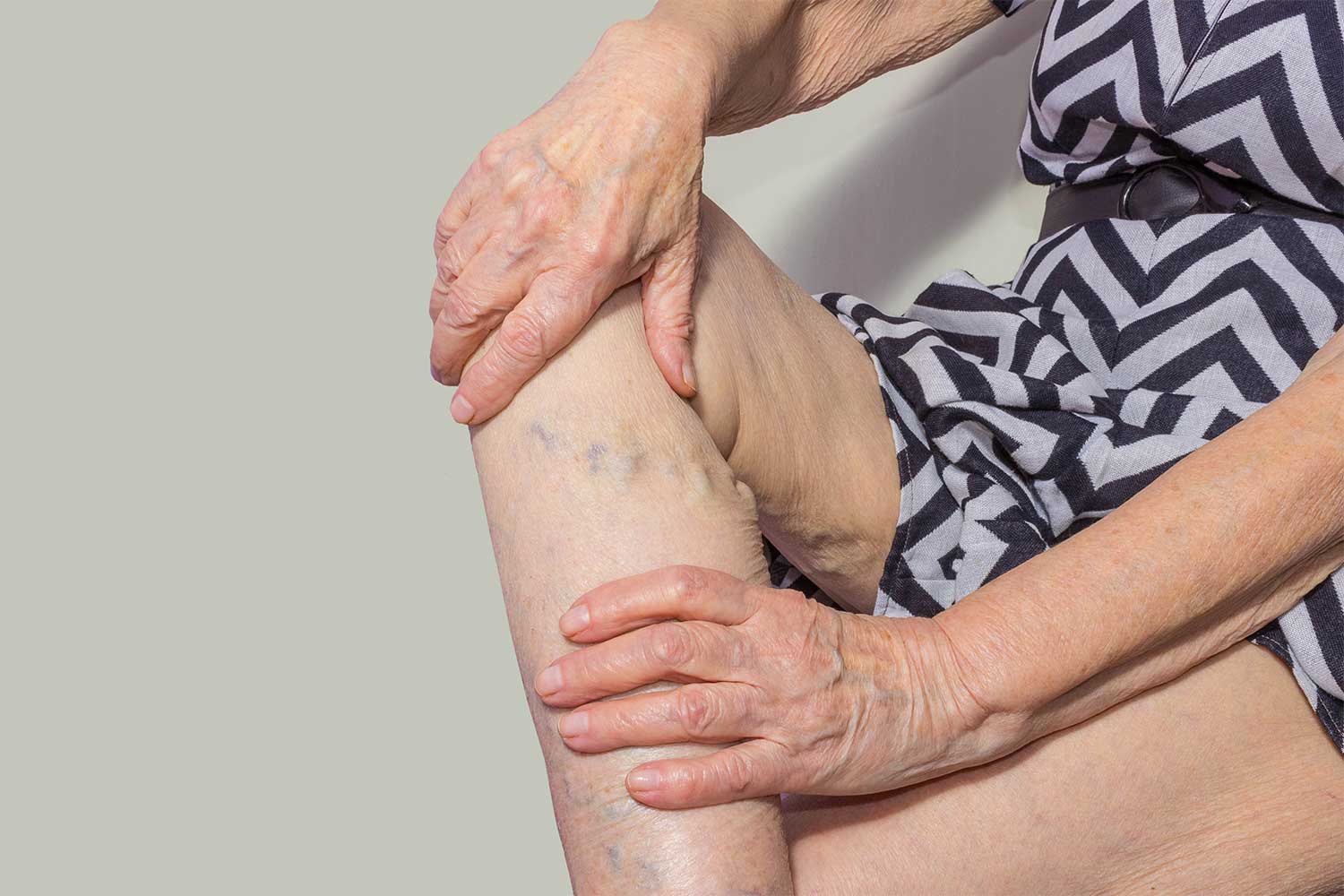
To look at varicose veins, you may think it’s possible for them to bleed externally quite easily. They appear as a web of vessels quite full of blood. Sometimes the skin can seem stretched to the limits trying to contain them, and you can see the darkness of the accumulated haemoglobin inside.
However, it is actually quite rare for varicose veins to bleed externally. Read on to find out why, and how you can care for your condition, or the varicose veins of a client or loved one.
What causes varicose veins to bleed externally?
Usually, bleeding from varicose veins only occurs in the rare case where an elderly patient may have neglected the symptoms of worsening chronic varicose veins over a significant period of time.
The good news is, by understanding varicose veins, you can control the condition. By getting a diagnosis and treatment plan as early as possible, you make it more than likely the varicose veins can avoid cases of external bleeding.
What do varicose veins look like?
Varicose veins occur when the one-way valves and walls of the veins weaken, causing a back-flow of blood, pooling, and causing the vein to enlarge. Visually, varicose vein disease looks like dark blue or purple veins that bulge in the legs, ankles and feet. These dark veins are usually accompanied by the feeling that the legs are unusually heavy. Other sensations include aches, throbbing pain, burning sensation, swelling of the lower part of the legs, and muscle cramps.
If you notice these symptoms in yourself, or in someone you know, it’s important that you seek treatment as soon as possible. When severe varicose veins are left untreated, they can lead to further health complications.
What are the adverse health conditions associated with varicose veins?
Increased pain, swelling/oedema, fatigue, and restless leg syndrome are some of the earliest conditions associated with varicose veins. If left untreated, more advanced conditions associated with varicose veins can develop. These include venous ulceration (where the skin barrier breaks down, usually around the ankle), venous eczema/dermatitis, hyperpigmentation (discolouration of the skin to a brown as the leaked blood disperses in the skin tissue), and lipodermatosclerosis (where the thickening of the skin and tissue of the lower leg or ankle usually implies chronic presence of varicose veins).
Lipodermatosclerosis can be the precursor for diseases of the lower leg including phlebitis (severe inflammation) and cellulitis (infection). Thrombophlebitis may also happen, when the varicose veins form blood clots.
How severe does a case of varicose veins have to be before external bleeding can happen?
Generally, only neglected cases of severe or chronic varicose vein disease will lead to external bleeding. Even so, this is quite a rare occurrence. External bleeding may happen when the veins are so distended and left untreated despite severe symptoms, they can form “blebs” in the lower legs and ankles. A “bleb” refers to a rounded outburst, or bubble that occurs due to the back-flow of blood.
These blebs are capillaries on the surface of the skin, and they can burst if they are knocked, scratched, or in circumstances of extreme pressure and heat (like a long time in a sauna or very hot shower).
How to prevent varicose veins getting worse
In order to prevent further debilitating complications from varicose veins, it is important to diagnose and treat at the first signs.
This is where carers, family and friends can be vital in supporting an older person to seek treatment for severe varicose veins.
Look out for signs of blue or purple veins in the legs. Listen out for signs of tiredness, heavy legs, restless legs, and pain in the lower legs as well.
Key Takeaways
- It is quite rare for varicose veins to bleed externally and may only arise in patients who have long-neglected treatment of severe varicose vein disease.
- Learn more about treatments available for moderate and severe varicose veins.