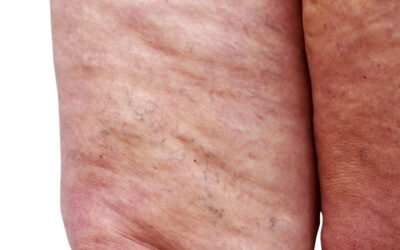
When discussing the vascular system, a lot of jargon can be thrown around. Superficial veins is a medical term that may confuse many patients and doctors alike. What does superficial mean and how do superficial veins become varicose?
What are Superficial veins?
Superficial veins is an umbrella term for veins that are close to the skin surface and are of varying diameters. You may be able to see them with the naked eye but in some cases, they are hidden within the fatty tissue and within compartments, lymph nodes, or muscles. Superficial veins are predominantly involved in thermoregulation but are important for redirecting blood from the capillary networks of the skin and soft tissue, into the deep veins, which then transport blood back to the heart.
The most clinically important hidden superficial vein of the lower leg is arguably the Great Saphenous Vein. This vein may be implicated in up to 80% of the vein problems we see in our practice. The Great Saphenous Vein lies within the saphenous compartment, a fibrous sheath in the thigh that protects the vein from the muscle below and the skin/soft tissue above.
Other important hidden superficial veins include perforators, pelvic veins, venous malformations such as the lymph node venous network (LNVN), and persistent embryological veins.
Can varicose veins form in superficial veins of the lower legs?
Yes. Veins all feature one-way valves on their inside walls. The movement of blood within veins must occur in one direction only. The valves within superficial veins prevent blood from returning backward and pooling.
Due to genetics or other factors like standing for extended periods of time or injury, if prone, these valves can fail. This makes the blood pool and leaks backward in the faulty area of the vein and it becomes incompetent at efficiently transporting blood back into the deeper veins and ultimately back to the heart.
This can happen to both the surface superficial veins and the deeper superficial veins like the Great Saphenous Vein. Surface superficial varicose veins are those that can be seen either as visible blue/red or green veins on the skin surface or as large bulging veins protruding out from the skin.
People are often motivated to have their visible superficial veins treated because of the painful symptoms (pain, throbbing, swelling, itching, etc.) and aesthetics of the veins, and discover they have deeper superficial varicosities too. An ultrasound ordered by the phlebologist is mandatory in these situations and will help clarify the full extent of the problem.
Treatment for superficial veins.
When superficial veins have become faulty and poor at returning blood to the heart (varicose veins), they will not right themselves without medical intervention.
For the very superficial varicose veins, your phlebologist (vein doctor) may use either sclerotherapy or in some cases ambulatory phlebectomy. Sclerotherapy involves injecting a sclerosant into the visible vein, which irritates the interior of the vein, it closes and heals over. This may be done under the naked eye following a comprehensive ultrasound.
For the more internal superficial veins, such as the Great Saphenous Vein, they may use endovenous laser ablation, radiofrequency ablation, or cyanoacrylate closure (VenaSeal, Vein Glue). Endovenous laser ablation is probably the most popular of the techniques and involves inserting a laser fibre into the problem vein and thermal closure of the vein under local anaesthetic.
For more information, please discuss these treatments with Dr Paraskevas at your initial consultation.
Key Takeaways
- Superficial veins may be situated on or just under the skin surface or slightly deeper within the fatty tissue and within superficial compartments.
- Varicose veins can form in all forms of superficial veins.
- Treatment may include sclerotherapy, endovenous laser ablation, radiofrequency ablation, or Vein Glue.